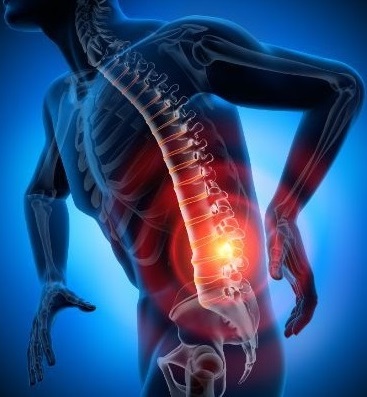
Lumbar laminectomy is revealed as an essential answer for those experiencing spinal stenosis, a painful condition that affects the spinal canal in the lower region of the spine.
Spinal stenosis, characterized by the narrowing of this vital canal, can cause a variety of symptoms, including persistent lower back pain and discomfort in the lower limbs. In this context, lumbar laminectomy is an advanced and effective surgical approach designed to provide patients with a path to relief and restoration of quality of life.
CONTENT:
- What is Lumbar Laminectomy?
- Performing the Procedure: Step by Step
- Recovery and Benefits of Lumbar Laminectomy
- Conclusion: A Solution with Bright Prospects
What is Lumbar Laminectomy?
Lumbar laminectomy is a surgical procedure that involves removing a portion of the bones called the laminae from the back of the lumbar vertebrae. This strategic intervention is primarily aimed at creating additional space in the spinal canal, removing pressure on the nerves and spinal cord. In essence, laminectomy paves the way for these delicate structures to regain their freedom and function within normal parameters.
Performing the Procedure: Step by Step
1. Preoperative Assessment: Confirming and Elaborating the Diagnosis
Before starting the intervention, the patient undergoes a thorough preoperative assessment. This includes laboratory tests, advanced medical imaging such as computed tomography or magnetic resonance imaging, and a detailed discussion with the specialist. The purpose of this stage is to confirm the diagnosis of spinal stenosis, to identify the anatomical peculiarities of the affected region and to establish a personalized surgical plan.
2. Anesthesia: A State of Comfort for the Patient
After the preoperative assessment is complete, the patient enters the operating room, where general anesthesia is administered. This procedure ensures that the patient is completely asleep and does not feel pain during the operation. Maintaining a comfortable position throughout the procedure is essential for as smooth a recovery as possible.
3. Access to the Spine: Surgical Incision
With the patient under general anesthesia, the surgeon begins the procedure by making an incision in the lumbar region. Surgeons make this incision precisely to allow access to the affected vertebrae and ensure adequate visualization of the intervention area.
4. Removing the Slats: Creating the Necessary Space
With access secured, the surgeon uses specialized instruments to remove small segments of bone called lamellae. This step is crucial for creating additional space in the spinal canal, thereby eliminating excessive pressure on the nerves and spinal cord.
5. Nerve Release: Reducing Pressure and Correcting Abnormality
Removing the lamellae allows the surgeon to identify and correct any pathological tissue changes that may be contributing to the spinal stenosis. The pressure on the nerves and spinal cord is significantly reduced, facilitating the recovery of these sensitive structures.
6. Closing the Incision: Toward Completion of the Procedure
At the end of the lumbar laminectomy, the surgeon carefully closes the incision with surgical sutures. Furthermore, this step is essential to ensure proper wound healing and to minimize the risk of infection.
Through this meticulous, step-by-step approach, lumbar laminectomy becomes an effective surgical option for patients seeking relief from spinal stenosis. Carefully and precisely carrying out each step of the procedure is important to ensure optimal results and a recovery as fast and comfortable as possible.
Recovery and Benefits of Lumbar Laminectomy
After the lumbar laminectomy is completed, a crucial stage of the medical process begins: the patient’s recovery. This period can vary depending on the complexity of the surgery and the health of each individual, but the tangible benefits of laminectomy often become apparent during and after this recovery phase.
Recovery from a lumbar laminectomy can take an average of 4 to 6 weeks, but the exact time can vary depending on the complexity of the procedure and the individual patient’s progress.
After such surgery, patients can start walking quite quickly, often even in the first days after the operation. However, returning to normal activities and walking without support may take several weeks.
-
Improvement of Symptoms
Many patients experience significant improvement in symptoms immediately after surgery. Lumbar pains that were initially present may diminish or even disappear, and sensations of tingling or weakness in the lower limbs may experience a considerable improvement. This development brings a sense of relief and comfort, giving the patient a much improved quality of life.
-
The role of Physiotherapy
Physiotherapy often becomes an essential component of the recovery process. Specialized exercises and techniques guide patients to strengthen the muscles around the spine, improve posture, and regain flexibility. These physiotherapy sessions aim to reinforce the results of the surgical procedure, ensuring a full recovery and preventing the recurrence of symptoms in the future.
-
Returning to Moderate Activities
As the patient progresses in recovery, it is recommended to gradually resume moderate activities. Even though rest is essential for the first few weeks, once the doctor deems it safe, the patient can gradually return to normal daily activities. This can include walking, swimming, or other light physical activity that supports spinal strength and flexibility.
-
Postoperative monitoring
After the back operation, it’s crucial to keep checking the patient’s health regularly. Additionally, seeing the doctor regularly helps check how well you’re recovering and adjust any advice about exercise or treatment.
-
Improving the Quality of Life
Over time, lumbar laminectomy helps improve the quality of life. It allows patients to move better and do daily tasks without ongoing pain and discomfort, regaining their independence.
Conclusion: A Solution with Bright Prospects
Lumbar laminectomy is emerging as an effective surgical option, offering relief and hope to patients affected by spinal stenosis. However, decide after discussing with your specialist, considering benefits, and respecting risks. In light of medical advances, lumbar laminectomy is thus becoming a gateway to an improved quality of life for those dealing with this complex condition.