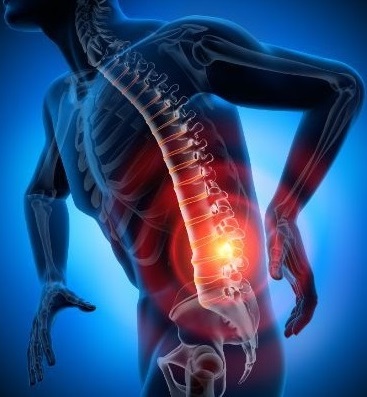
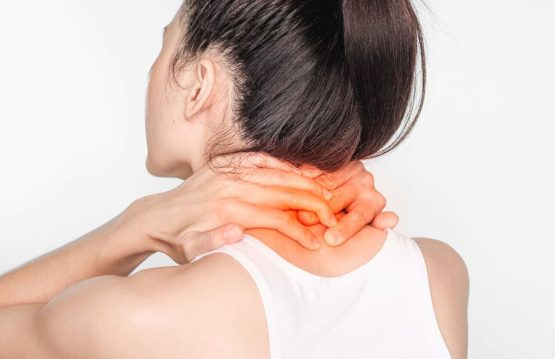
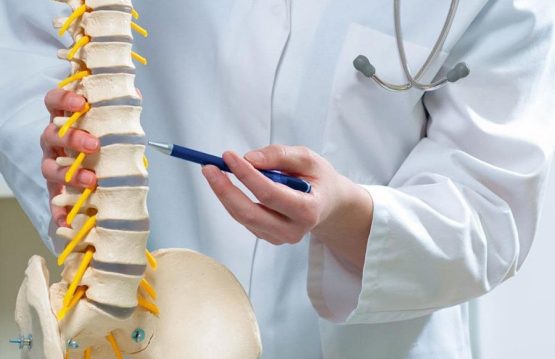
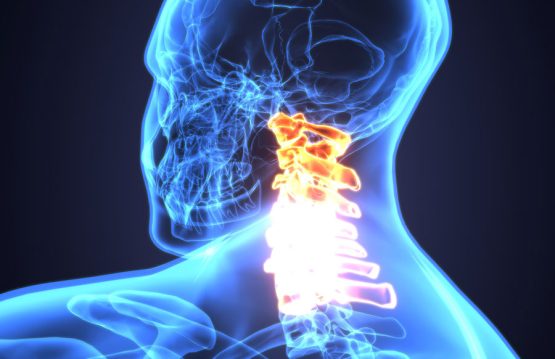
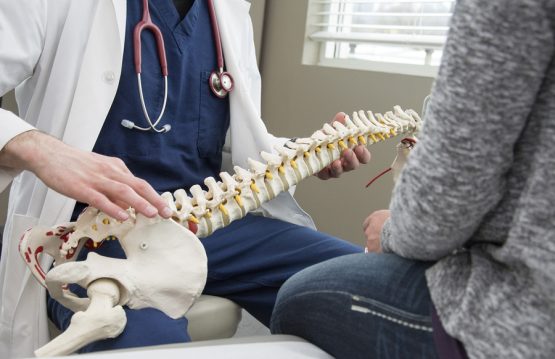
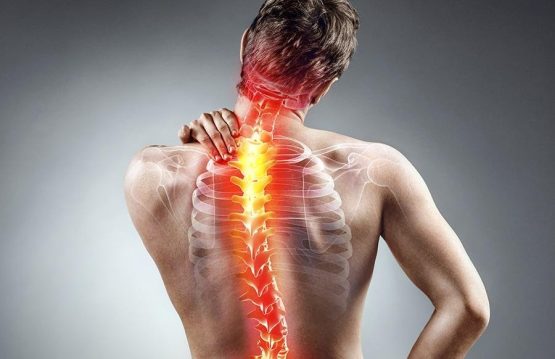
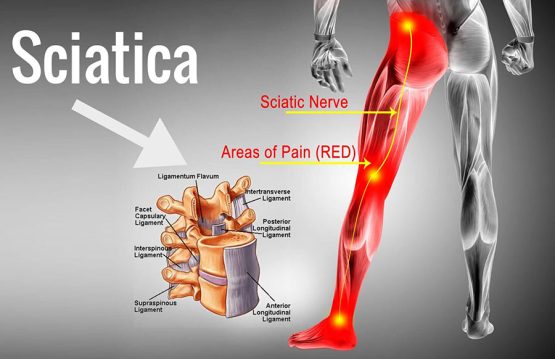
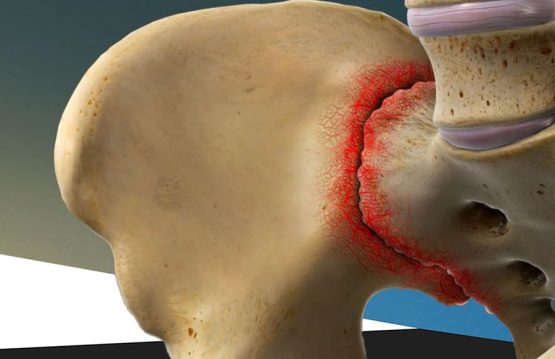
Sprains and strains are common injuries that affect muscles and ligaments. Most can be treated at home without seeing a primary care physician.
What is the difference between sprain and strain? The ligaments, muscles, or tendons that line the bones and wrists can be affected if the movements we make are not correct (sudden or violent movements of the bones).
Sprain
It consists in the violent stretching of the articular ligaments, but without a rupture or tearing. Sprain occurs in the ankle, knee or wrist.
We recognize a sprain after painful swelling, the movements can be done, but they are not natural and even bruises can occur.
Until he arrives at the hospital, the wounded man can be given ice packs or we can immobilize his area by wrapping it with an elastic bandage or bandage. At the hospital he will be consulted by a specialist doctor and an X-ray will be taken.
The treatment of the sprained ankle consists in putting a bandage or a splint for a period of 2 weeks or in the most painful case it is put in plaster.
Strain
It means moving a bone in the joint. The dislocation receives the name of the region in which it occurred: shoulder, foot, elbow.
Strain occurs by falling on the shoulder, elbow, foot (by landing from the jump on the outer edge of the foot). It is more common in athletes (sports injuries) and tourists.
First aid in case of strain of the foot is done by pulling the foot as it is done when removing the boot, the knee must be in flexion to allow relaxation of the Achilles tendon. Arriving at the hospital, he was received by a medical specialist.
CONTENT:
Causes of Sprains and Strains
The movements of the ankle and knee joints, performed suddenly and forcing the physiological limits of the body, can cause a minor trauma, by stretching the ligaments that connect the bones of the foot and those of the leg. In critical cases, the inversion, the most common cause of sprain, is generated by rotating the ankle inward, simultaneously with bringing the sole of the foot inward.
An even more painful form of a sprain is caused by twisting the upper ligaments and those outside the calf. External rotation and abduction of the ankle lead to sprain by eversion, a form of trauma that may require surgery. Most often, you can have the unpleasant experience of a sprain on a walk in the mountains, due to choosing the wrong pair of shoes, or on the football field, during a man-to-man dribble.
Symptoms of Sprains and Strains
The intensity of the symptoms depends on the severity of the lesions. The first symptom of a sprain is pain, although the painful sensation may occur with some delay after the injury, because the inflammatory process takes time. It is not excluded that the moment of ligament overload is not aware.
Local pain and tenderness, but also exacerbation of painful sensations when mobilizing the joint are specific symptoms of sprains. Swelling of the affected area is sometimes associated with bleeding in the ligaments. Deep bleeding is associated with bruising of the skin, but it can take up to 24 hours for it to become apparent.
The combination of pain and swelling of the joint causes the body to protect the injured area, which leads to functional difficulties through self-preservation. Sprains located at the ankle or knee are associated with a limited ability to move the joint, its mobilization being associated with intense pain.
In some situations, all these symptoms may be associated with a numbness, and in the case of severe sprains, at the time of occurrence, it is possible to hear or feel, when mobilizing lightly, a joint click (a crack).
Treatment of Sprains and Strains
Simple forms of sprain can be treated at home. In their case, it is necessary to immobilize the injured area and avoid forcing it. It is sometimes necessary to rest for a few days and limit the usual activities, which put pressure on the affected joint.
Ice packs are useful. They are kept on the joint for about 10-15 minutes, four to eight times a day. It is also useful to massage with an ice cube on the joint, through circular movements.
Compression of the joint is useful in reducing inflammation. Elastic bandages can be used on the affected area and on the extremities to prevent distal inflammation. The compressive bandage soothes pain, but should not be excessively tight, uncomfortable or disrupt blood circulation. Also to reduce the inflammation of the limb with the affected joint, it must be kept high, at a height above the patient’s heart.
In more severe cases, in which the ligaments have been partially torn, it is necessary to immobilize the ankle with a cast of plaster or orthosis. The time required for healing is set by the orthopedist. For very severe sprains, with torn ligaments, associated with bleeding, surgery is required.
Therapy should not be limited to reducing pain, reducing edema and eliminating bruising, but should be continued after the acute phase is over, with medical gymnastics and physiotherapy, so that the affected joint is restored to normal parameters or as close as possible to the condition before injury.
The recovery protocol is necessary to reduce the sensitivity of the joint, but also in order to prevent recurrence, whose risk is relatively high, which can lead to motor deficit or a compensatory position that causes, over time, other postural disorders. It is important to know that the pain passes before the affected joint is completely restored, and medical gymnastics is essential for complete healing.
Manual therapy is recommended especially in case of severe sprains and recurrences or after periods of immobilization. It is important to say that these joint injuries, especially in the knee, are considered favorable factors for osteoarthritis.
Regardless of the severity of the sprain, it is recommended to consult a specialist, in order to benefit from a correct evaluation and personalized therapeutic indications.
The duration of recovery depends on the severity of the sprain. In mild cases, it can last one to two weeks, while in more severe cases, it can reach 10-12 weeks. Surgical repairs, necessary for completely torn ligaments, have the longest recovery period and are followed by postoperative therapy.
The presentation to the doctor is absolutely necessary, if the symptoms worsen after the application of cold compresses and compression of the joint, with elastic band, the second or third day after the trauma.