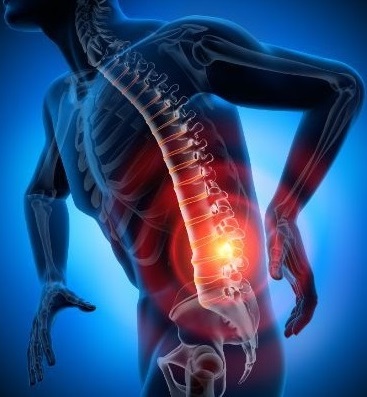
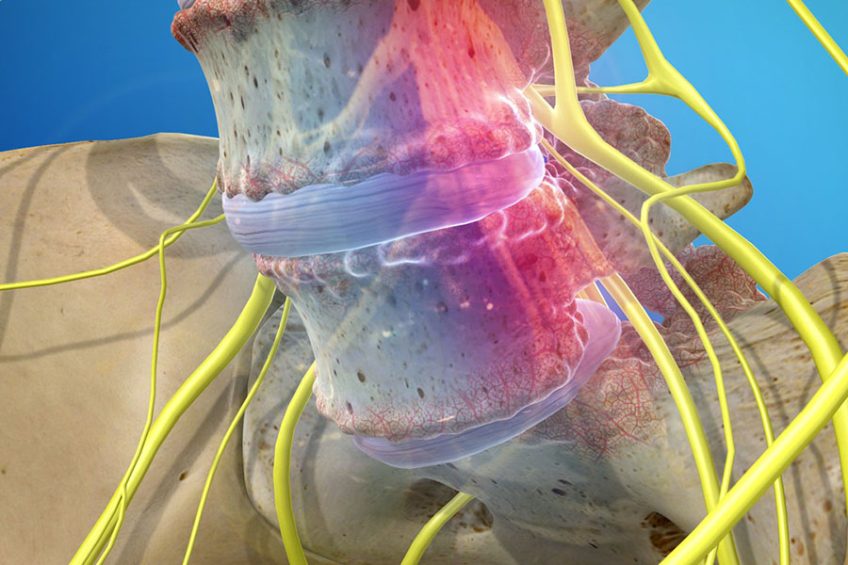
Spondylolisthesis is the anterior slip of one vertebra to the rest of the vertebrae, more precisely the vertebra changes its initial position and leaves the alignment of the other adjacent vertebrae.
Spondylolisthesis is classified according to the causes of its occurrence and is of five types: congenital, isthmic, degenerative, traumatic and pathological.
CONTENT:
Causes
- congenital defect in the spine (usually occurs a few years after birth);
- acute trauma to the back;
- exaggerated repetitive extensions (common in certain sports);
- muscle atrophies;
- degenerative diseases of the spine.
Symptoms
Other people suffer from pain, especially under stress and during certain movements. The pain caused by spondylolisthesis can spread from back to front in a belt shape. There is also a feeling of instability in the spine.
Especially in the morning, when the back muscles are relaxed, the pain is strong. In severe cases, there are reflex, sensory and motor disorders, which can extend to the legs. These symptoms occur when the vertebra squeezes a nerve root through a spondylolisthesis.
However, there are no specific gliding symptoms, as the symptoms may be similar to those of other back problems, such as herniated discs.
In the congenital form of patients with spondylolisthesis, usually the symptoms are mild or mild, being a slow progressive process. So the nerves have the opportunity to adapt to changed circumstances.
Treatment
Physical and rehabilitation therapy
It should not be initiated until after a period of rest and once the pain with daily activities has diminished. Physical regimens reduce the stress by extension of the lumbar spine and promote a nonlordotic position. It consists of exercises for stretching the abdominal muscles, wearing harnesses and strengthening the lumbodorsal fascia.
Thoracolombosacral orthosis trimming provides relief for those who do not respond to rest or whose daily activities cause symptoms. This type of rod is effective for patients with less than 50% slip. The stem is worn for 3-6 months. If the slip is below 50% but the patient is symptomatic, non-interventional therapy is recommended: stretching exercises, antilordotic rod, modification of activities. If the pain continues, spinal fusion is recommended.
Surgical therapy
Surgery is indicated for immature skeletal patients with slipping over 30-50% because they are at risk of progression with neurological deficit and persistent pain. If the pain does not resolve in 6-12 weeks with rest and immobilization, surgery is recommended. Spondylolysis with low-grade spondylolisthesis can be treated noninterventionally.
Intervention options include direct repair of spondylolytic defect, fusion, reduction and fusion, and vertebrectomy. The best results are seen in patients with lithic defect. Disc degeneration is a relative contraindication. Slips over 2 mm decrease the success of surgical repair.
In situ fusion at the affected level is the standard criterion for surgical treatment for most patients in whom conservative therapy fails. In situ fusion is recommended for patients with low-grade, persistent, symptomatic spondylolisthesis and for those who are not candidates to repair the defect.
Decompression and fusion are performed in cases of hard compression in the presence of intestinal or bladder dysfunction or significant motor deficits. Decompression is never performed without concomitant fusion. Fixing the pedicles with screws allows rapid mobilization and early ambulance after decompression and fusion. Fixation can be beneficial in repairing pseudoarthrosis and preventing progressive slipping.
The reduction of spondylolisthesis is performed by the closed or open procedure. The reduction serves to correct the lumbosacral kyphosis and decrease the sagittal translation. Vertebrectomy can be used to treat spondyloptosis and as an alternative to reduction or fusion in situ. The postoperative rate of neurological deficit is 25%