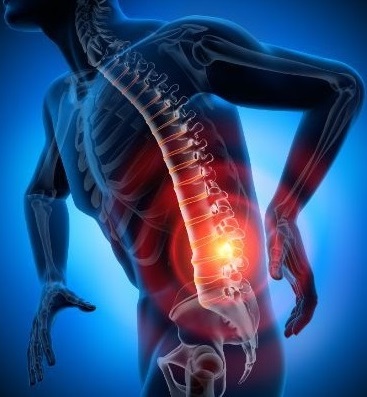
Disc protrusion is a common spinal condition that can cause pain and discomfort for those affected. To better understand this problem, it is important to examine the anatomy of the spine and understand what exactly constitutes a disc protrusion.
The spine comprises a series of bones known as vertebrae, which are separated by intervertebral discs. These discs consist of a sturdy outer ring called the annulus fibrosus and an inner gelatinous substance known as the nucleus pulposus. They serve as shock absorbers and allow fluid movement of the spine.
Disc protrusion occurs when the gelatinous inner part of the intervertebral disc begins to protrude from the annulus fibrosus. This can be caused by various reasons, such as trauma, the natural wear and tear of the disc over time, or an incorrect body position that puts pressure on the disc.
CONTENT:
Symptoms of Disc protrusion
The symptoms of a herniated disc are diverse and can vary considerably depending on the location and size of the herniation, as well as the level of pressure exerted on nerves or other surrounding structures. These symptoms can affect a person’s quality of life and ability to carry out normal daily activities. Here are some common symptoms of a herniated disc:
1. Localized and radiating pain
Pain is a characteristic symptom of a disc protrusion. This sensation can manifest as sharp, dull, persistent pain, or discomfort in the affected spinal area. The pain may radiate to other parts of the body, such as the legs or arms, depending on the level of the hernia and the affected nerves. For example, a lumbar disc herniation can cause pain that radiates down one or both legs, known as sciatica.
2. Muscle weakness and abnormal sensations
The pressure exerted by the herniated disc on the nerves can cause abnormal sensations such as tingling, numbness or burning sensations in the affected area. Muscle weakness in the area may also occur. For example, in the case of a cervical disc protrusion, these abnormal sensations can be felt in the arms and hands.
3. Limitation of mobility
A disc protrusion can affect the normal mobility and flexibility of the spine or surrounding regions. Affected individuals may experience difficulty performing specific movements, such as bending or turning the body, without experiencing pain or discomfort.
These symptoms can vary in intensity and can appear suddenly or develop gradually over time. It is important to pay attention to early signs and seek medical attention if symptoms persist or worsen. Early diagnosis and treatment can help manage symptoms and prevent long-term complications associated with a herniated disc. A doctor or health professional can recommend additional tests and an appropriate treatment plan to effectively manage this condition.
Diagnosis of Disc protrusion
Diagnosing a herniated disc involves a series of steps and investigations performed by doctors or health professionals to identify and confirm the presence of this spinal condition. Disc protrusion can be diagnosed after a careful evaluation of symptoms, physical examination, and imaging investigations. Here’s how the diagnostic process typically works:
-
Medical history and physical exam
The doctor will take a detailed history to understand the patient’s symptoms, how they have evolved and how they affect quality of life. A comprehensive physical examination will evaluate mobility, muscle strength, reflexes, and sensation in the affected areas.
-
Assessment of symptoms
The diagnostic process takes into account common symptoms such as localized or radiating pain, muscle weakness, and abnormal sensations. Details regarding the duration, intensity, and how the symptoms affect daily activities are essential for the physician in formulating an accurate diagnosis.
-
Imaging investigations
Medical imaging is essential in confirming the diagnosis of disc protrusion. These investigations may include:
X-rays: Can give a picture of the bone structure and rule out other conditions of the spine, but do not give precise details about the intervertebral discs.
MRI (magnetic resonance imaging) or CT (computed tomography): These imaging methods provide clearer and more precise details of the intervertebral discs, nerves and surrounding tissues. MRI is more commonly used to evaluate the disc and nerves, providing detailed images in different planes of the spine.
-
Other additional tests
Occasionally, healthcare professionals might require additional tests like electromyography (EMG) or nerve conduction tests to assess nerve function and ascertain if the herniated disc is exerting pressure or impacting the nerves.
Correct diagnosis of disc protrusion is crucial to develop an appropriate treatment plan. After confirming the presence of a herniated disc, the doctor might suggest various treatment options, including physical therapy, medications, injections, or, in severe cases, surgery. It is important to seek specialist medical attention for the evaluation and proper management of disc protrusion, given that each patient may require a personalized approach depending on their clinical characteristics and the severity of the condition.

Treatment of Disc protrusion
Treatment for disc protrusion is variable and may involve a combination of conservative methods and medical or surgical interventions, depending on the severity and location of the problem.
Here are some of the treatment options for a herniated disc:
Rest and activity modifications
Relative rest and avoidance of activities that aggravate pain are often recommended initially. Maintaining proper posture and avoiding movements or positions that put pressure on the spine can help reduce symptoms.
Physical therapy
Exercise and movement therapy are essential in the management of disc protrusion. The physical therapy program may include back strengthening exercises, stretching, and correcting posture to reduce pressure on the affected disc.
Medications
Healthcare providers may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen to reduce inflammation and pain. They might also recommend pain relievers to manage discomfort. Muscle relaxants could be prescribed in some cases to alleviate muscle spasms associated with a herniated disc.
Alternative therapies
Some people find benefits in complementary therapies such as acupuncture, chiropractic or massage therapy. These treatments can help relax the muscles and relieve the pain associated with the herniated disc.
Epidural injections
Epidural corticosteroid injections may help reduce inflammation and pain in the affected area by administering them near the affected disc or irritated nerve.
Surgery
In severe cases or when conservative treatments do not bring relief, surgery may be an option. Surgery may involve removing the part of the bulging disc that is putting pressure on the nerve or other surrounding structures. Surgery can be performed through various procedures such as discectomy, laminectomy or microdiscectomy.
It is important to note that each case of disc protrusion is unique and requires an individualized approach to treatment. Before starting any treatment program, it is essential to consult a doctor or health professional to obtain an accurate diagnosis and develop an appropriate treatment plan.
Also, adopting a healthy lifestyle that includes regular exercise, maintaining a healthy weight, and avoiding positions or movements that can strain the spine can help prevent or reduce the risk of a herniated disc.