Shoulder pain can significantly affect a person’s quality of life and can be caused by a variety of factors. From injuries and inflammation to chronic conditions or poor posture, this pain can have multiple origins.
In this article, we’ll explore common causes of shoulder pain and effective treatment options to restore mobility and comfort.
CONTENT:
Causes of shoulder pain
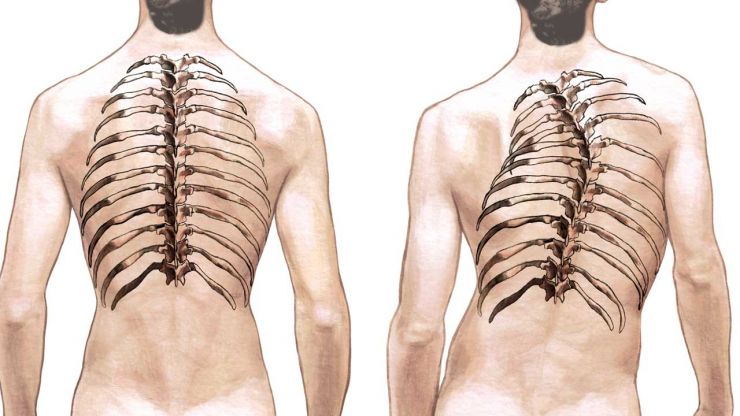
The shoulder, a complex and mobile joint, can often be affected by persistent pain, affecting daily activities and quality of life. The causes of shoulder pain are varied and can include traumatic injuries, inflammatory conditions, as well as wear and tear associated with the natural aging process.
In this context, it is crucial to understand how various conditions can affect the shoulder and identify appropriate treatment modalities.
-
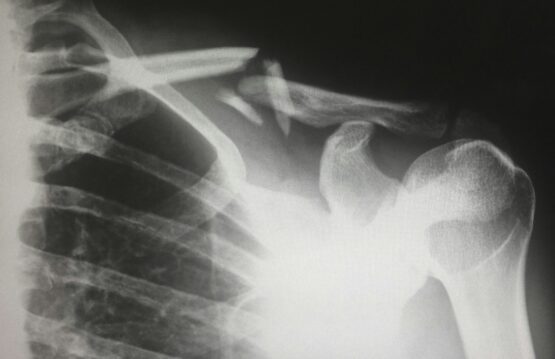
Traumatic injuries
Bumps or falls can cause injuries to the shoulder joint, such as sprains, muscle strains or even fractures. These injuries can trigger intense pain and require immediate medical attention.
-
Tendinitis
Inflammation of the tendon around the shoulder joint, known as tendinitis, can cause pain and discomfort. Overuse, repetitive movements or improper positions can contribute to the development of this condition.
-
Bursitis
The bursa, a small piece of tissue inside the shoulder that facilitates smooth movement, can become inflamed, causing bursitis. This can occur due to overuse or injuries.
-
Adhesive capsulitis (frozen shoulder)
This condition characterized by progressive stiffness and pain in the shoulder joint can occur for no apparent reason. Although the exact causes are not always clear, it can be associated with inflammation or minor trauma.
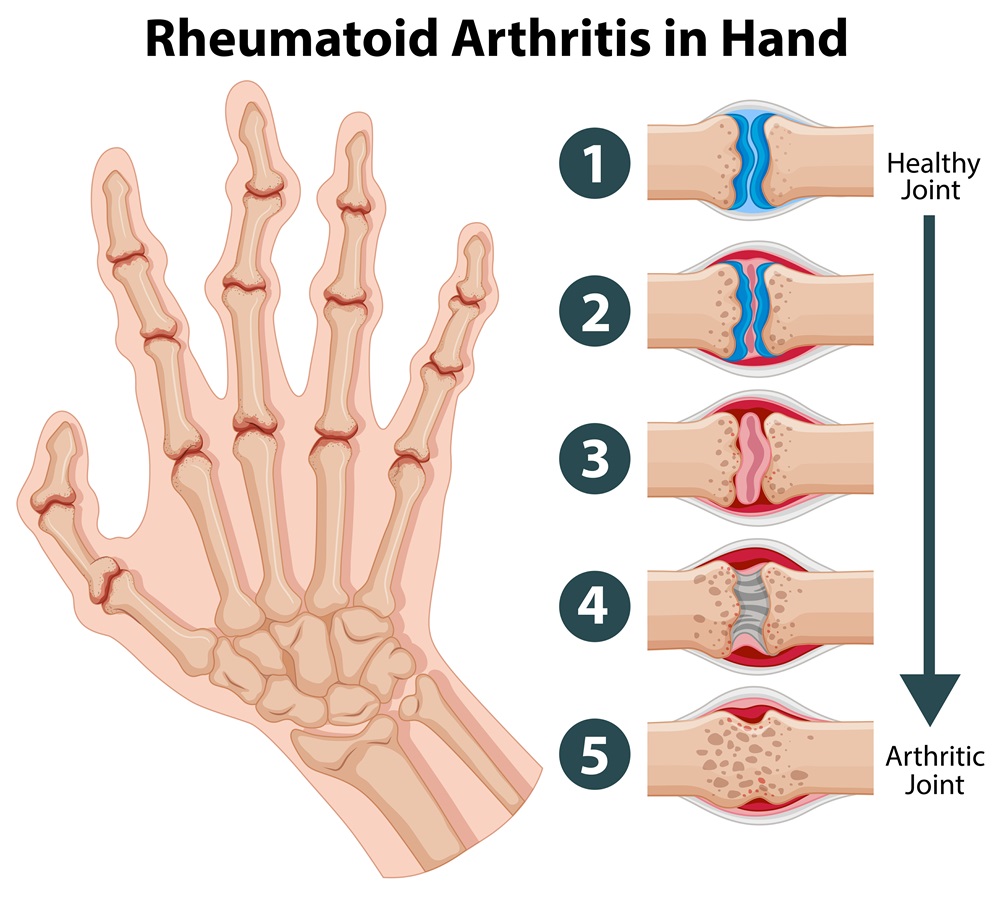
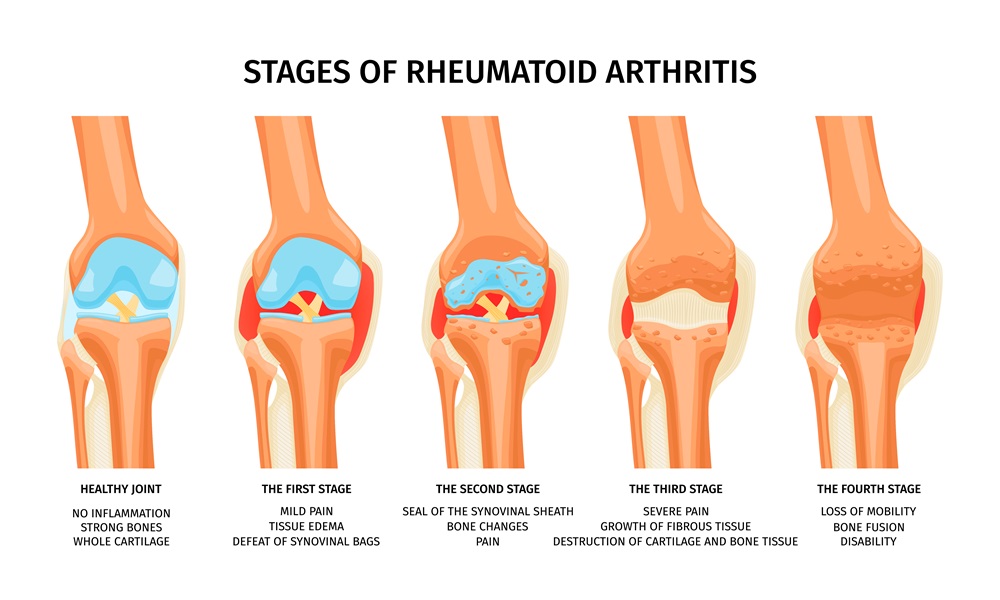
Shoulder osteoarthritis, a form of cartilage wear and tear, can cause persistent pain. This can be the result of aging, overuse, or medical conditions such as rheumatoid arthritis.
-
Cervical nerve compression
Nerves in the cervical area can be compressed, leading to pain in the shoulder and arm. This compression can have various causes, including disc herniation or spinal stenosis.
Effective treatment for treating this pain
Shoulder pain can have a significant impact on everyday life, limiting mobility and causing persistent discomfort. In the search for an effective treatment, the comprehensive and personalized approach becomes essential to restore the functionality of the joint and reduce unpleasant symptoms.
In this context, varied treatment strategies can cover a wide range of options, from conservative methods to more invasive medical interventions.
-
Rest and reduction of activity
With a recent injury or inflammation, consequently, rest can be essential for healing. Reducing activity and avoiding movements that cause pain can help reduce discomfort.
-
Physical therapy
A customized physical therapy program can be effective in restoring mobility and strength to the shoulder. Regular exercises under the supervision of a therapist can help restore the functionality of the joint.
-
Medication
Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to reduce inflammation and pain. Prescription pain management medications may also be an option depending on the specific cause of the pain.
-
Infiltrations with corticosteroids
For persistent inflammation, corticosteroid injections into the shoulder joint can provide rapid relief and help manage symptoms.
-
Surgery
For severe injuries or conditions that do not respond to conservative treatments, however, surgery may be an option. This may involve repairing tendons, removing inflamed bursae, or other specific interventions.
-
Stretching and strengthening exercises
The exercise program recommended by the physical therapist may include specific activities to stretch and strengthen the muscles and tendons around the shoulder.
-
Acupuncture and alternative therapies
Some people find benefits in alternative therapies, such as acupuncture or massage, in managing shoulder pain. However, it is important to always talk to your doctor before trying such treatments.
Conclusion
Shoulder pain can have multiple causes, and the optimal treatment depends on the correct diagnosis and the particularities of each case. Before beginning any treatment regimen, it is crucial to consult a medical professional for proper evaluation and guidance.
With the right approach and commitment to recommended treatments, many people can regain shoulder function and regain quality of life.