COVID-19 infection is proving to be much more than a respiratory illness. It can affect many organs, not just the lungs – from the skin and muscles to the eyes, heart and kidneys – creating long-term health problems. These include fatigue, blurred vision, difficulty breathing, muscle aches, confusion, headaches and even hallucinations.
Most people infected with the new coronavirus tend to have mild to moderate forms of the disease and heal within a few weeks. In contrast, people who survive COVID-19 infection after needing intubation and longer hospitalization may be left with a number of long-term side effects.
CONTENT:
- Long-term effects of COVID-19 infection known to date
- Long-term side effects – a feature of other viral infections
Long-term effects of COVID-19 infection known to date
Although there is still much to learn from people who have recovered from COVID-19, there are a number of long-term effects that doctors have seen so far.
Lung problems
We know that COVID-19 infection primarily attacks the lungs, causing inflammation. For this reason, survivors may experience long-term breathing difficulties. Some people recovering from COVID-19 may experience a dry cough or pain when breathing, and patients who have needed mechanical ventilation may have more severe symptoms.
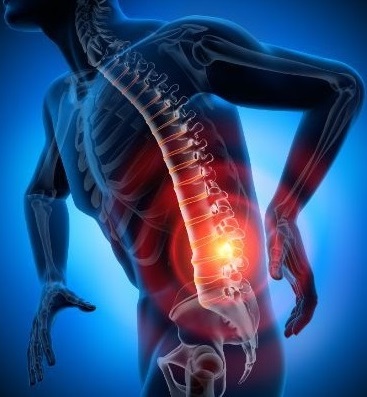
Along with the lung pain, there is discomfort in the back area. You shouldn’t be surprised that once you get in touch with the virus, your back starts to hurt.
Neurological problems
Research shows that COVID-19 infection can affect the brain and central nervous system. Some people who have recovered have reported symptoms such as headaches, dizziness, difficulty concentrating or memory, and even hallucinations. Researchers say that these symptoms are more common in patients who have had severe forms of the disease.
Heart problems
A study by Frankford University in Germany showed abnormal heart rates in more than 75% of those studied who recovered from COVID-19. It was found that a considerable majority of patients in the study had inflammation of the heart and mucous membranes. This can be disturbing, as inflammation of the heart can lead to long-term heart disease.
As we are dealing with a relatively new disease, it is not yet known why certain patients experience one or more side effects after infection with the new coronavirus, how long these effects persist and whether COVID-19 infection will cause certain chronic diseases. , who will need lifelong monitoring.
Long-term side effects – a feature of other viral infections
Long-term symptoms of a severe viral illness are not new. Infections with other pathogens are associated with long-lasting symptoms, from heart problems to chronic fatigue. Even common illnesses, such as the flu and pneumonia, can lead to a long recovery. For example, the flu has long been linked to persistent symptoms, such as fatigue and muscle aches.
Infections with certain bacteria and Zika virus, among others, are linked to Guillain-Barre syndrome, a condition in which the immune system attacks the nervous tissue, causing muscle weakness and paralysis.
There is a precedent for infections with other coronaviruses. For example, the first SARS coronavirus and the Middle East Respiratory Virus (MERS) caused serious illness, and a significant number of patients developed acute respiratory disease syndrome (ARDS) and needed intensive care.
Canadian researchers found common issues among SARS survivors in Toronto: sleep disorders, fatigue, depression, and muscle aches. One-third of survivors were forced to change jobs and lifestyles, and only 14% had no long-term symptoms. A Korean study found that 48% of MERS survivors experienced chronic fatigue within a year of recovery.
Many severe COVID-19 patients require a long recovery period, as widely recognized in the medical community. The virus can attack the heart through direct invasion and inflammation, damaging or destroying heart cells and affecting function. Also, the virus disrupts ACE2 receptors, which protect heart cells and degrade angiotensin II, a blood pressure-raising hormone.