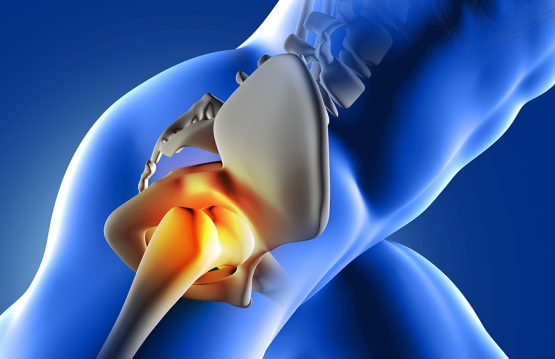
Jade therapy is an extraordinary solution even for those who suffer from advanced disc herniations when the pain goes down on the leg as well as for those in sciatica or lumbago crisis. It is the most performing system globally and offers a profound therapeutic experience. From a therapeutic point of view, it combines a very wide range of principles:
- Acupressure
- Thermotherapy
- Mechanical elongation of the spine
- Massage
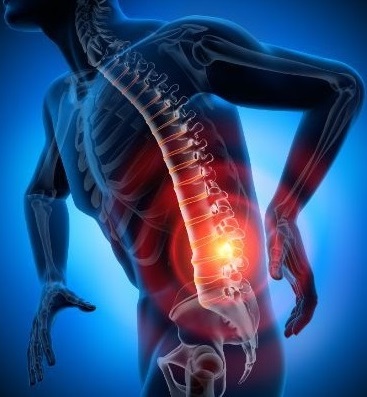
Back pain is pain in any region of the back. It is divided into cervical, thoracic back pain, lower back pain (lumbar) or sacral pain. Additionally, the lumbar region is the most prevalent area for pain as it primarily supports the weight of the upper body.
Episodes of back pain can be acute, sub-acute, or chronic, depending on the duration. Moreover, back pain is one of the most common reasons why people go to the doctor and one of the leading causes of disability worldwide. Most people have back pain at least once in their lifetime.
Jade bed therapy does not require any effort on the part of the patients. A session with this device lasts 45 minutes. Furthermore, a package of 10-12 sessions is recommended for long-term results. Additionally, it is mandatory to consume 250-400 ml of water before the procedure and 250-400 ml of water immediately after the procedure.
The only contraindication for this device is that there is no metal rod implant in the spine.

CONTENT:
- How does jade therapy work for back pain?
- How an automated Jade massage bed works
- Combining elongation procedures with spine toning procedures
- Benefits of Jade Therapy
- Warning
How does jade therapy work for back pain?
Jade therapy for back pain is based on the principles of heat and pressure therapy. Additionally, this can be done by various methods:
- Jade stone massage: The therapist may use smooth, pre-heated jade stones to massage painful areas of the back. Furthermore, the heat from jade stones relaxes tense muscles and can help reduce inflammation and discomfort.
- Jade wraps or compresses: Jade stones can be heated and placed on the affected area or wrapped in cloth to create compresses applied directly to the back. Additionally, this process can help warm the tissues, relax the muscles, and relieve pain.
- Jade Therapy Pads: There are devices that use jade therapy pads that can be applied to the concerned back. They are designed to emit heat and relax painful areas.
How an automated Jade massage bed works
The action of the massage bed comes in two directions:
1. Mechanical elongation of the spine as a therapeutic principle
All 7 programs, by reducing the rolls of paravertebral jade, along the spine, according to the natural curvature of the spine, achieve mechanical elongation of the spine with the effect of decompressing the intervertebral discs and increasing the spaces between the vertebrae.
2. Long-term, infrared radiation therapy (Far-Infrared Technology) as a therapeutic principle
Throughout the 7 massage programs, they heat the jade rolls, either based on your personal choice or as per the specialist’s recommendation, to temperatures between 50 and 70 degrees Celsius.
All programs use infrared thermotherapy (heat) and all programs stimulate and improve blood circulation, calming and completely eliminating the symptoms of poor circulation, contributing to a strong detoxification on all 5 pathways, relaxes muscles, eliminates inflammation in the body and contributes strongly to pain therapy, eliminating it.
Combining elongation procedures with spine toning procedures
Through the automated massage bed with Jade therapy, we obtain the elongation of the spine, decompression, and repositioning of the vertebrae. Now, we should ask ourselves why the spine got into the situation where it needed mechanical intervention to eliminate back pain.
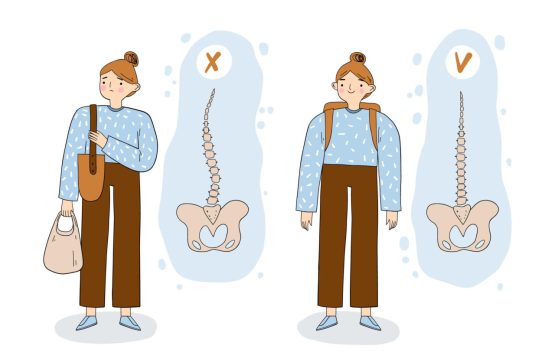
In most cases, sedentary lifestyle, overweight and atrophy of the back muscles are the causes that generate these episodes of back pain.
Given that most of you lead a sedentary lifestyle and your daily routine lacks physical activity, heading to the gym may not be the ideal solution for spinal health. Engaging in weightlifting exerts pressure on the spine, potentially causing vertebral compression over time. Furthermore, improperly executed exercises can have lasting adverse effects on the spine.
Benefits of Jade Therapy
- Deep muscle relaxation
- Stimulating and improving blood circulation
- Better oxygenation of muscles, tissues, brain
- Elimination of insomnia
- Elimination of emotional problems: depression, panic attacks, anxiety
- Elimination of BURN OUT syndrome – chronic fatigue, exhaustion, stress
- Elimination of headaches
- Elimination of menstrual pain
- Elimination of back pain
- Hot spine elongation
- Elimination of joint pain
- Elimination of rheumatic pain
- Deep detoxification
- Elimination of chronic constipation
- Hormonal balance
Warning
Even though jade therapy may help some individuals with back pain, it’s crucial to talk to a doctor or therapist before trying any alternative treatment. Also, make sure it’s safe for your health and avoid using jade stones on irritated or damaged skin.