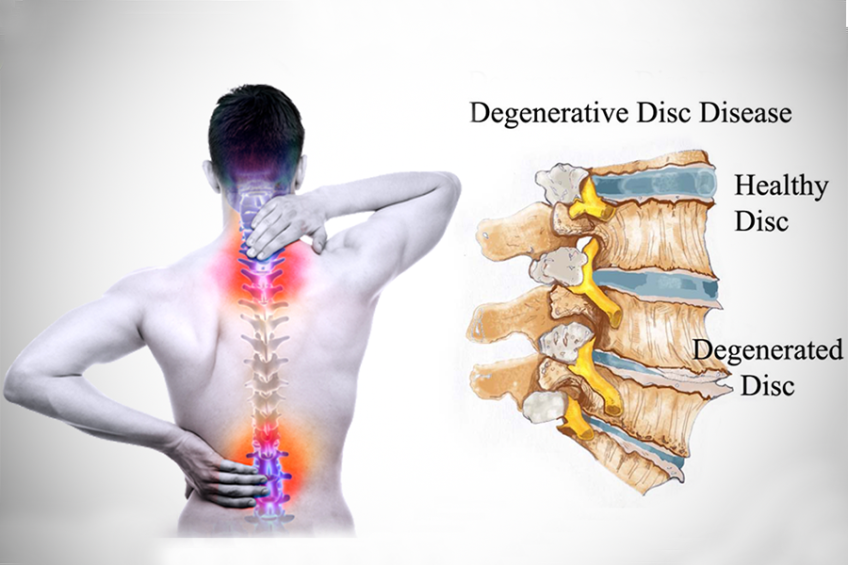
Degenerative disc disease is a combination of symptoms associated with aging that may worsen with age. Degeneration of the vertebral discs is not necessarily followed by physical manifestations, such as low back pain radiating to the legs, neck pain (neck pain), muscle weakness or numbness of the limbs.
The intervertebral discs connect the vertebrae of which the spine is composed and are composed of a fibrous and resistant outer ring and an elastic gelatinous tissue located in their center. These discs act as a “shock absorber”, giving the spine protection from shocks caused by large or sudden movements, such as jumping, lifting weights or running.
CONTENT:
Causes of Degenerative Disc Disease
Aging is the main factor that causes degeneration of the intervertebral disc. Thus, in the elderly patient there are two phenomena that contribute to the deterioration of the quality of the intervertebral disc:
Loss of water content of tissues, which leads to thinning and loss of elasticity of the disc, with increased compression by the vertebrae
Formation of microruptures in the fibrous ring (external portion of the intervertebral disc), caused by all the demanding movements performed during life / minor injuries accumulated over time.
However, the degenerative process of the disc can be accelerated by many factors, including:
- Injuries – can lead to rupture of the intervertebral disc (fibrous ring) and herniated disc
- Nutritional factors – obesity promotes degeneration of the intervertebral disc
- Mechanical factors – intense physical activity, incorrect exercise or demanding physical work (eg weightlifting) accelerates the degradation of the disc, by exerting additional pressure on it
- Genetic factors – alteration of the expression of certain genes (responsible for the synthesis of structural components, degradation enzymes or the expression of some receptors) can play a decisive role in the degeneration of the intervertebral disc. (1, 3, 4, 5, 6)
Degenerative Disc Disease symptoms
Degenerative disc disease may be asymptomatic in some patients, while in others there is severe pain that can affect their quality of life. Usually, the symptoms worsen with age, when complications occur, such as osteoarthritis, which is manifested by back pain and stiffness.
The most common and early symptom of degenerative disc disease is back pain radiating to the thighs and legs. Other events include:
- tingling or numbness in the lower limbs
- neck pain that extends to the shoulders, arms or hands
- muscle spasms in the lumbar or cervical area
- pain in a sitting position, when lifting or twisting
- periods of severe pain, which decreases after a few days or weeks
- weakness in the hands or feet (especially at the ankles)
- inability to lift the leg
Pain specific to degenerative disc disease may worsen when sitting, bending over, or when the torso is turned. Usually, walking and lying down in a lying position help to relieve pain.
What exactly happens and how does this condition occur?
- Discs dry out and shrink – made of about 80% water, as they age they slowly lose water. This loss of flexibility puts more pressure on the ring.
- Small holes appear in the annular space – sometimes part of the gel material (or nucleus pulposus) comes out through a rupture in the wall and touches the nerves. (Herniated disc)
- This material has many inflammatory proteins that can inflame the nerves and cause pain. These ruptures also affect the nerves in the fibrous ring and small movements, called micro-movements, which can cause discogenic pain. Over the years, the proteins eventually dry out and the discs become stiffer; In many people, this leads to less pain when they are around the age of 60.
- Disc space becomes smaller – due to water loss in the discs, the distance between the vertebrae begins to collapse, which is why they are shorter as we age.
- Abnormal bone growth – without the discs holding the vertebrae apart, they can rub against each other causing abnormal bone growth.
- The spinal canal narrows – the stress of all the above changes causes the ligaments and joints of the facets to enlarge (hypertrophy), as they try to compensate and spread the load over a larger area. This overgrowth forces the spinal canal to narrow, which can compress the spinal cord and nerves that cause pain (spinal stenosis).
The symptoms of degenerative disc disease vary from person to person. Many people with injuries have no pain, while others may have pain so intense that it interferes with their daily activities.
Today the disease affects people over the age of thirty, although the first signs of degenerative disc disease of the cervical spine often appear in adolescence.
Treatment of Degenerative Disc Disease
The goal of treatment is to relieve symptoms and reduce the progression of the disease as much as possible.
In most cases, healthcare providers recommend conservative treatment, which includes:
- physical therapy – regular exercise that strengthens the muscles of the back, in order to reduce pressure on the spine
- medication – non-steroidal anti-inflammatory drugs (eg aspirin, ibuprofen) help reduce local inflammation and relieve pain. In more severe cases, healthcare providers may prescribe stronger painkillers.
- epidural infiltrations with corticosteroids (steroidal anti-inflammatory drugs)
If symptoms persist despite conservative treatment (minimum 3 months after initiation), healthcare professionals may suggest surgery (in 5% of cases).
There is a surgical indication for degenerative disc disease:
- in patients with severe spinal stenosis
- if the pain is persistent, refractory to conservative therapy
- in situations where the symptoms do not subside or improve after a period of 6-12 months from the initiation of non-surgical treatment